Flatfoot Surgery (Pes Planus) - treatment for painful, progressive flatfoot deformity
Flatfoot surgery is a specialist option for people with painful, progressive flatfoot deformity that has not improved with appropriate non-surgical care. Flatfoot (also called pes planus) describes a foot posture where the arch is lowered, and the heel may drift outwards, changing how the foot loads during walking. Many flat feet are painless and need no treatment. Surgery is usually considered only when the condition becomes symptomatic—causing persistent pain, fatigue, instability, or difficulty with footwear and activity.
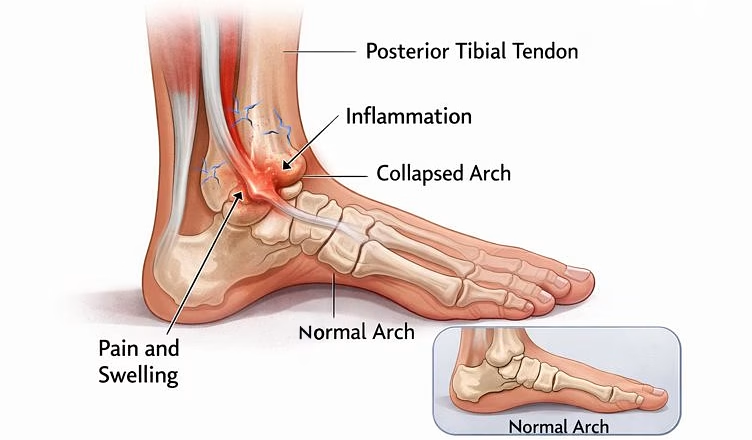
What causes a painful flatfoot?
Flatfoot can be flexible (the arch reforms when non-weight-bearing or on tiptoes) or rigid (stiff and fixed). In adults, one of the most common causes of a painful, progressive flatfoot is posterior tibial tendon dysfunction (often referred to as progressive collapsing foot deformity). The posterior tibial tendon helps support the arch; when it becomes inflamed, stretched, or torn, the arch can gradually collapse, and the hindfoot can drift into valgus (heel rolling outward).
Other causes can include:
- Long-standing flexible flatfoot with increasing symptoms over time
- Arthritis in the hindfoot or midfoot joints
- Previous injury, ligament laxity, or fracture malalignment
- Inflammatory conditions that affect joints and tendons
A careful assessment is essential because “flatfoot” is an umbrella term, and the most appropriate treatment depends on the underlying cause.
Symptoms that may suggest surgery is needed
People considering flatfoot surgery often report:
- Pain along the inside of the ankle/arch (often tendon-related)
- Pain on the outside of the ankle due to impingement as the heel drifts outward
- Flattening that is worsening over time
- Swelling, fatigue, or a feeling of “giving way”
- Reduced walking tolerance and difficulty with uneven ground
- Trouble fitting supportive footwear comfortably
Non-surgical options first
Before discussing surgery, most patients are treated with a structured non-operative plan. This may include:
- Supportive footwear and activity modification
- Orthotics or ankle-foot bracing to support the arch and control heel position
- Physiotherapy focusing on calf flexibility, tendon strength, and foot control
- Anti-inflammatory measures when appropriate
If symptoms persist despite well-fitted support and rehabilitation, or if the deformity is progressing, flatfoot surgery may be considered.
Goals of flatfoot surgery
The main aims of flatfoot surgery are to:
- Relieve pain and reduce inflammation or impingement
- Restore more stable alignment of the heel and arch
- Improve function and walking endurance
- Prevent further collapse and joint damage where possible
Surgery is highly individualised. Many flatfoot reconstructions involve a combination of procedures rather than a single operation.

Common procedures used in flatfoot surgery
Your surgical plan depends on whether the foot is flexible or rigid, tendon integrity, joint condition, and severity of collapse. Options may include:
- Tendon procedures: cleaning (debridement) or reconstruction of the posterior tibial tendon; sometimes tendon transfer to support arch function
- Calcaneal osteotomy: shifting the heel bone to improve alignment and reduce strain on the arch structures
- Midfoot osteotomy or fusion: correcting collapse through the midfoot; fusion may be recommended if there is arthritis or instability
- Spring ligament or deltoid ligament reconstruction: when ligament support has failed
- Gastrocnemius recession or Achilles lengthening: addressing calf tightness that contributes to collapse and overload
- Arthrodesis (fusion) procedures: in rigid flatfoot or arthritis (e.g., subtalar or triple fusion) to correct alignment and relieve pain
A detailed consultation and weight-bearing imaging help determine which combination is most appropriate for your foot.
What to expect: assessment, surgery, and recovery
Assessment typically includes a clinical examination, gait assessment, and weight-bearing X-rays. Depending on your symptoms, an ultrasound or MRI may be used to assess tendon and ligament condition.
Flatfoot surgery is usually performed under regional or general anaesthetic and often involves a period of protected weight-bearing. Recovery varies based on the procedures performed, but it commonly includes:
- A phase of immobilisation in a cast or boot
- A staged return to weight-bearing
- Physiotherapy to restore strength, mobility, and balance
- Gradual return to footwear and activity as healing progresses
Swelling can take several months to settle, and full recovery is often measured in months rather than weeks, especially after reconstruction or fusion.
Why choose a specialist team?
Flatfoot reconstruction is complex, and success depends on accurate diagnosis, correct alignment goals, and a well-structured rehabilitation plan. A specialist team will assess whether surgery is truly needed, discuss realistic outcomes, and tailor the procedure to your lifestyle and activity demands.
If flatfoot pain is limiting your walking, sport, or work, I can assess the cause of your symptoms, guide you through non-surgical options, and explain whether flatfoot surgery or reconstruction is appropriate.
