Plantar Fasciitis Surgery - next steps for persistent, chronic heel pain
Plantar fasciitis surgery is only considered when persistent heel pain has not improved with a structured programme of non-surgical treatment. Plantar fasciitis is one of the most common causes of heel pain and typically presents as sharp pain under the heel, often worse with the first steps in the morning or after rest. Most people improve with conservative care, but a small proportion develop chronic symptoms that significantly limit walking, work, or sport. In these cases, plantar fasciitis surgery may be discussed as a next step.
What is plantar fasciitis?
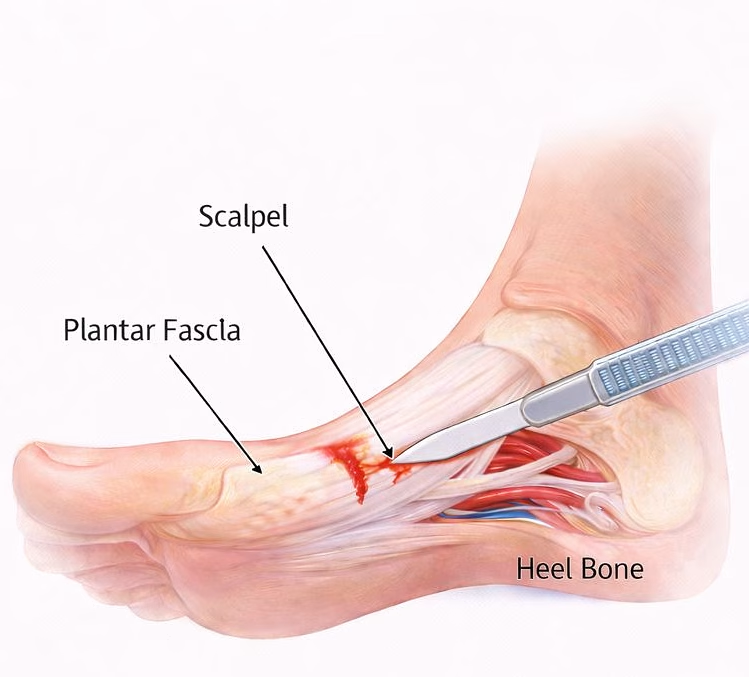
The plantar fascia is a thick band of tissue that runs along the bottom of the foot from the heel to the toes. It helps support the arch and absorbs load during walking and running. In plantar fasciitis, the fascia becomes painful where it attaches to the heel bone (calcaneus). Despite the “-itis” name, long-standing cases are often more degenerative than purely inflammatory, which is why rest alone may not resolve it once it becomes chronic.
Symptoms of plantar fasciitis
Typical symptoms include:
- Pain under the heel, often on the inside (medial) side
- “First-step” pain in the morning or after sitting
- Pain that eases as you warm up, then worsens after prolonged standing or activity
- Tenderness when pressing the heel attachment point
- Tight calf muscles or Achilles tendon stiffness
Because other conditions can mimic plantar fasciitis (such as nerve entrapment, stress fracture, or fat pad pain), specialist assessment is important—especially if symptoms are atypical or not responding to treatment.
Non-surgical treatments are tried first
Before considering plantar fasciitis surgery, most patients undergo a stepwise plan that may include:
- Calf and plantar fascia stretching (often the cornerstone of treatment)
- Supportive footwear and heel cushioning
- Insoles or orthotics to reduce strain and improve mechanics
- Activity modification and load management
- Night splints in selected cases
- Physiotherapy and strengthening for foot/ankle control
- Ultrasound-guided injection in some cases (with careful discussion of risks/benefits
- Shockwave therapy (ESWT) where appropriate
Surgery is usually reserved for symptoms that persist—often for many months—despite consistent, well-directed conservative management.
When is plantar fasciitis surgery considered?
Plantar fasciitis surgery may be discussed when:
- Pain has lasted for a prolonged period and remains severe
- You have tried appropriate conservative care without sufficient improvement
- Symptoms are significantly restricting walking, work, or exercise
- Imaging and clinical assessment support plantar fascia pathology and exclude other causes
The aim is to select patients carefully to maximise the chance of meaningful, lasting improvement.

What to expect: assessment, surgery, and recovery
Assessment typically includes a detailed history and examination, and, when the diagnosis is unclear or the symptoms are complex, imaging such as ultrasound or MRI.
After plantar fasciitis surgery:
- You may be placed in a boot or post-operative shoe
- Weight-bearing guidance varies depending on the procedure and surgeon preference
- Swelling and heel tenderness can persist for weeks, with gradual improvement
- Physiotherapy may be advised to restore flexibility, strength, and walking mechanics
- Return to running and high-impact sport is usually staged and depends on healing and symptom response
Most patients aim to return to comfortable daily walking first, followed by a gradual return to higher activity levels.
Types of plantar fasciitis surgery
The most common surgical option is plantar fascia release (also called partial plantar fasciotomy). This involves releasing a portion of the plantar fascia near its heel attachment to reduce tension and pain. It may be performed through an open approach or endoscopically, depending on the surgeon and the case.
In selected cases, additional procedures may be considered at the same time, such as:
- Gastrocnemius recession (calf muscle lengthening) if calf tightness is a significant contributor
- Addressing other contributing problems identified on assessment, such as nerve irritation or biomechanical overload
I will explain the rationale for the recommended approach and whether a release, calf procedure, or alternative strategy best suits your presentation.
Risks and considerations
As with any procedure, plantar fasciitis surgery carries risks. These may include infection, nerve irritation, persistent pain, arch discomfort, or slower-than-expected recovery. Your surgeon will discuss the specific risks relevant to your foot, overall health, and the procedure planned.
Why choose a specialist team?
Plantar fasciitis is common, but chronic heel pain is not always straightforward. A specialist assessment ensures the diagnosis is correct, conservative options have been optimised, and surgery—if needed—is matched to the true driver of pain.
If heel pain has become long-standing and limiting, we can assess your symptoms, confirm whether plantar fasciitis is the cause, and discuss whether plantar fasciitis surgery or other targeted options are appropriate.
